The second national survey of patient safety specialists: what’s changing for people in the role?
Background
Since 2020, all NHS organisations in England have been required to appoint at least one patient safety specialist. Originally set out in the 2019 NHS Patient Safety Strategy, the role is intended to provide leadership across an organisation, coordinating efforts to improve safety and drawing on the latest thinking about how to ensure patients are safe.
Between 2022 and 2024, THIS Institute undertook an initial evaluation of the patient safety specialist role, which included a national survey of patient safety specialists. We wanted to fully understand what the role is supposed to be in theory – and how it works in practice. We published our findings in journal articles and in a blog that provided a snapshot of patient safety specialists, their work, and their hopes for the role.
Thanks to funding from the National Institute for Health and Care Research (NIHR), we’re now following up this evaluation with a larger-scale study, which will finish in 2028. The second study continues to track the work of patient safety specialists and also looks at a complementary role, the patient safety partner (patients, carers and members of the public who work with NHS organisations to provide their own distinctive perspective on patient safety). As part of this evaluation, we have completed a follow-up survey of patient safety specialists. Carried out between July and September 2025, the second survey took place just over two years after the first one.
Nearly 200 patient safety specialists completed that first survey, and a similar number completed the second survey (thank you to all who responded). The groups completing the two surveys may be different (we didn’t track individual patient safety specialists’ responses from one survey to the other) and so some caution in interpretation is needed. Still, looking at the surveys side-by-side gives us a valuable opportunity to see how things are changing for patient safety specialists. A further survey in 2027 will allow us to track their experiences over a four-year period.
The people

In demographic terms, the people who responded to the second survey look fairly similar to those who responded to the first. As might be expected, participants in the second survey had more experience than those in the first: 53 per cent have now been in patient safety specialist roles for more than two years (versus 29 per cent in the first survey), and nearly 25 per cent have been in the role for more than four years. This suggests that many patient safety specialists are staying in the role for the long run.
There are some indications that the numbers of patient safety specialists employed in organisations may be increasing – though these indications need to be treated with caution. Eleven per cent of respondents to the second survey said that there were seven or more patient safety specialists in their organisation (compared to 4 per cent in the first survey). Conversely, only 25 per cent of respondents to the second survey said they were their organisation’s only patient safety specialist (37 per cent in the first survey). This could represent a real expansion of the role as it has matured, or it could be due to different people responding to the survey. It could also be a result of roles being cut up differently, or of organisational mergers.
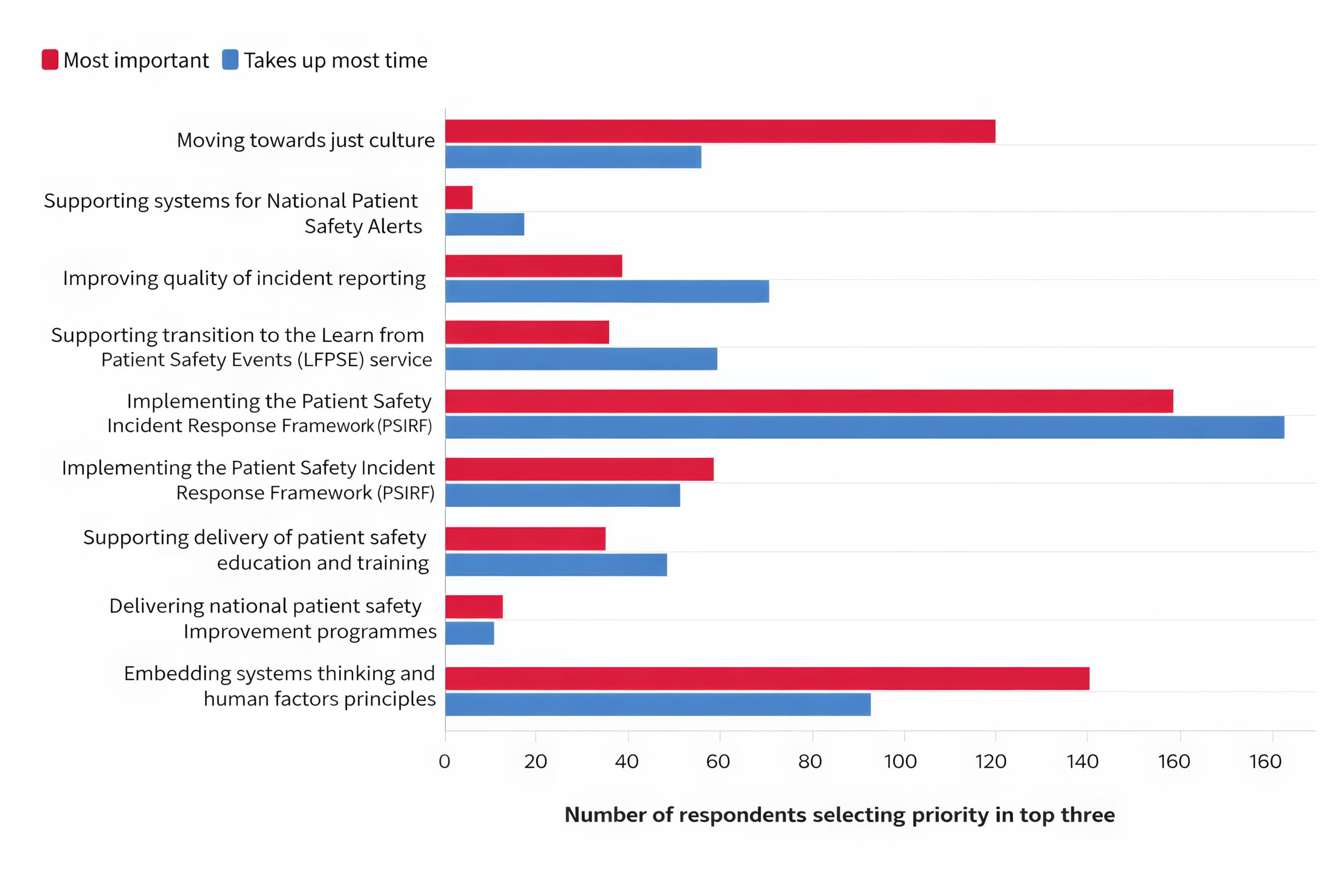
Figure 1: Priorities seen as among the top three most important and the top three most time-consuming
The leavers
A subset of participants in the second survey had moved on from their original role as a patient safety specialist, either to take up another patient safety specialist role (24) or to do a new job altogether (13). The numbers in this group are small, but of the 13 participants no longer in a patient safety specialist role, nine said that most or all of their new role was about patient safety and two said that some of it was about patient safety.
The reasons leavers gave for vacating their original roles were not always positive. Several indicated frustration as a factor, or wider issues in their organisation (Figure 2). In other cases, organisational restructuring resulted in changes to the role or redundancy. But leavers offered examples of achievements, too (Figure 3). In all, 52 per cent who had moved on, either to another patient safety specialist post or to a different role, who answered the question said that they would consider applying for another patient safety specialist role (15/29); eight were not sure and six said they would not.
Figure 2: Examples of reasons given for leaving the patient safety specialist role

Figure 3: Examples of biggest achievements cited by people who had left a patient safety specialist role

The role in practice

In the original survey, we asked participants to tell us their three most important priorities as a patient safety specialist, and the three things they spent most time on. The responses showed something of a disparity: patient safety specialists tended to indicate that major, strategic changes were most important, but this wasn’t where they were spending most time.
We repeated the question in the second survey, updating the response options using the most recent priority areas for patient safety specialists highlighted by NHS England. The results have changed a little from last time (Figure 1).
Implementing the Patient Safety Incident Response Framework (PSIRF) – a new approach to learning from patient safety incidents that seeks to maximise the usefulness of learning for improvement – remains one of the highest priorities, and the thing that takes up most time for our participants. Strategic objectives around improving systems and culture are still top priorities for patient safety specialists, and these still aren’t the things they spend the most time on – but this may be changing. For example, in 2023, 26 per cent of participants (46/180) put “moving towards just culture” among the three things they spend most time on, even though it was a top-three priority for many more. In 2025, “improving safety culture” was among the three things they spent most time on for 42 per cent of participants (66/157).
There’s clearly still a mismatch between what patient safety specialists spend their time on and what they see as a priority, but it looks like the gap may be closing. Again caution is needed, not just because the participants may be different but also because the wording used by NHS England is slightly different. It’s also not necessarily a given that there should be perfect alignment between top priorities and time allocation, and some of the other activities on the priority list have at least the potential to impact culture, directly or indirectly.
Even if the shift is real, it could suggest a few different things. Perhaps patient safety specialists as a whole are indeed able to spend more of their time on long-term strategic objectives. Or it might be that organisations that are committed to strategic change are investing in more patient safety specialist roles, or that patient safety specialists who aren’t able to find the time to do what they see as most important are leaving the roles. Our in-depth qualitative work, involving ethnographic case studies of the patient safety specialist and partner roles in six organisations, will help to shed more light on this.
Patient safety partners
The 2023 survey suggested that many patient safety specialists were not clear on the place of the new role of patient safety partner in their organisations, and the 2025 survey indicated that this had not shifted much. With all NHS provider organisations now required to appoint at least two patient safety partners, more work may be needed to clarify the role and the distinctive contribution it can make.
A new question, asked in 2025 only, also suggested a range of views among patient safety specialists on the extent to which close working between specialists and partners is important – again, producing a broad range of responses (figure 4).
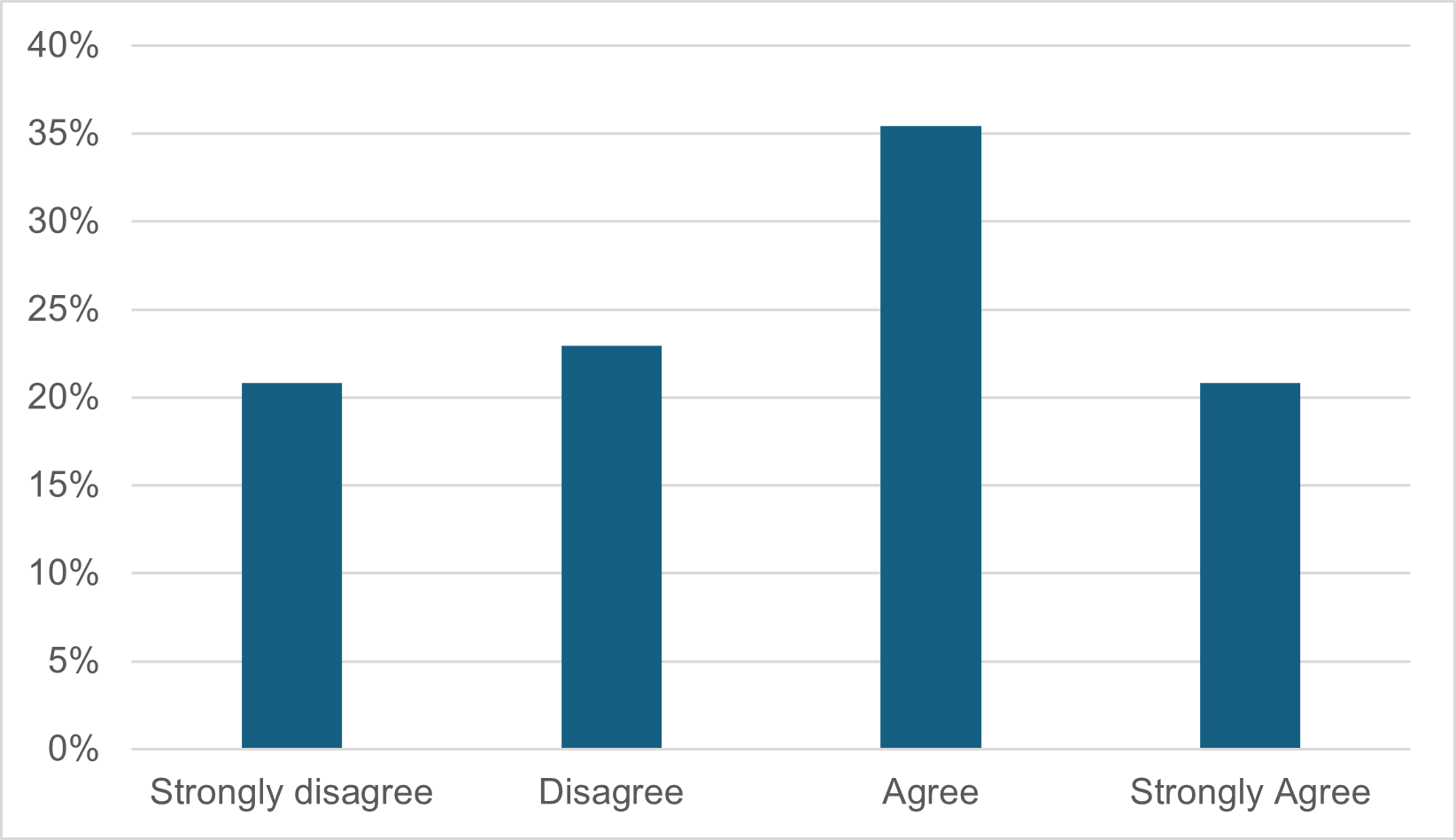
Figure 4: Proportions of respondents agreeing and disagreeing with the statement ‘Working closely with the Patient Safety Partner(s) in my organisation is vital to the success of my role’ in the 2025 survey.
What happens next?
The second survey provides a useful snapshot of how patient safety specialists are experiencing the role a few years in. The third survey in 2027 will help us understand how things continue to develop. As part of our NIHR funding, we have also launched our first survey of patient safety partners, which will help us learn more about how that group are experiencing their roles so far. We will follow up with them again in 2028.
The surveys are just one part of the wider study. We are also analysing data about the advanced patient safety training that specialists receive, reviewing similar specialised safety roles in other sectors, and carrying out in-depth ethnographic research of the work of specialists and partners in six NHS organisations. We’ll be sure to provide further insights from our study as they emerge.

