Clear, practical microlearning resources on governance and leadership in healthcare improvement. Includes key approaches across all levels, planning questions, and top tips to support improvement efforts.
Introduction
This resource offers clear, practical guidance on the key concepts of governance and leadership in healthcare improvement.
After reading this resource, you should be able to:
- Define governance and leadership and explain how they overlap
- Describe the interactions between governance and leadership at multiple levels across the healthcare system
- Explain how boards, leaders, and teams can create the conditions for improvement
- Describe effective leadership in healthcare improvement across systems and teams
- Apply eight key practical tips for governance and leadership to your work.
The resource also includes practical questions to guide planning, alongside links to further reading for deeper insights.
Whether you’re starting a new improvement initiative or looking to expand and sustain existing work, this guide provides actionable advice to support your efforts.
Definitions
Healthcare improvement requires strong governance and effective leadership. Governance and leadership are overlapping concepts with a complex relationship.
Together, governance and leadership shape the conditions in which improvement can thrive, influencing everything from strategic direction to day-to-day culture.
Governance
Governance involves the structures and processes that allow oversight, monitoring, and accountability within a system, shaped by formal and informal interactions between those working within that system.
It typically involves:
- Setting a long-term strategy to describe how the organisation’s values and priorities will be achieved.
- Ensuring accountability by monitoring and measuring performance.
- Shaping culture and systems to make sure long-term strategies and accountability work effectively.
Leadership
Leadership can be defined in many ways but is perhaps best summed up as the processes by which individuals or groups are enabled, encouraged, or inspired to achieve agreed goals within a given context.
Governance and leadership at multiple levels
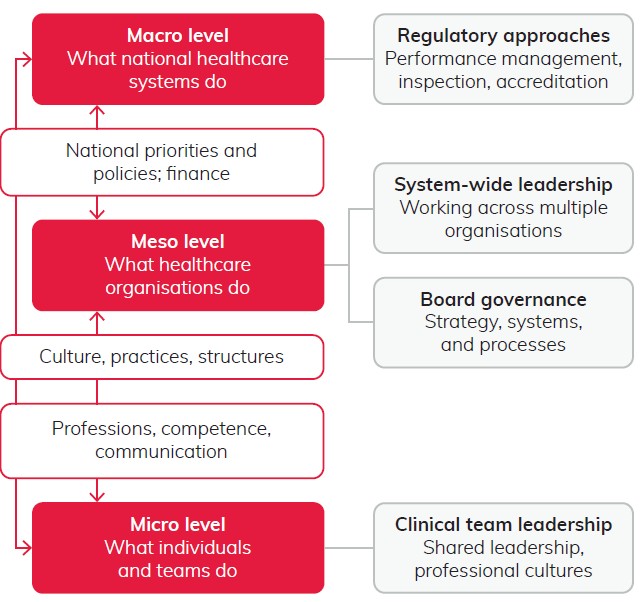
Governance and leadership operate at multiple levels – known as macro, meso, and micro – across the healthcare system. Understanding the interactions between these levels helps understand how healthcare can be improved.
At macro level – what national healthcare systems do
At the macro (national) level, a range of bodies may set policies, issue guidance, and allocate resources. Regulators may set standards and put processes in place to oversee them, such as performance management, inspection, and accreditation, taking action where needed.
At meso level – what healthcare organisations do
At the meso (organisational) level, board governance may try to influence national priorities and to influence within their own organisations.
At micro level – what individuals and teams do
At micro (team) level, clinical and corporate teams work together to deliver care, while responding to potential changes.
How do boards, leaders, and teams create the conditions for improvement?
Governance and leadership shape how improvement happens in practice. Boards, leaders, and teams can create the conditions for improvement at different levels of the system.
Boards
Boards comprise the senior leaders accountable for the quality and safety of care in the organisations they lead. Board governance plays a key role in quality and safety through:
- Setting clear, measurable goals aligned with national and local priorities.
- Ensuring members have a diverse mix of skills and experience.
- Involving stakeholders at all levels in shaping strategic priorities.
- Effective performance measurement and management.
- Using data to inform decisions and drive improvement.
Performance measurement
Performance measurement tracks how services perform against targets and standards. While it can improve care, it may also lead to box-ticking, where staff do just enough to achieve the target, or neglect harder-to-measure aspects like a person’s individual needs. One way of avoiding this is to give the performance measure an importance ranking so that people don’t cherry-pick the measure easiest to achieve.
Performance management
Performance management involves actively shaping performance, often based on available data. It can drive improvement but may also lead to unintended consequences, such as avoiding high-risk cases that could make performance seem worse. There is also a risk of ‘gaming’ targets, where services seek to improve only slightly on the previous year’s performance, to show superficial improvement.
Leadership approaches across systems and teams
Leadership has the potential to encourage and facilitate improvement (and the cultures associated with it) at every level. Effective leadership in healthcare improvement typically involves:
- Clearly understanding priorities, external drivers, and local issues.
- Influencing others – experience, technical expertise, extraversion, and conscientiousness are important characteristics for this.
- Engaging a wide range of stakeholders, even those resistant to change.
- Shaping team cultures and behaviours.
- Acting with integrity, fairness, and consistency.
- Recognising when change is needed and taking ownership.
At meso level
Different forms of leadership combine to play important roles in delivering major system change.
Clinical leadership is a ‘bottom-up approach’ that helps to ensure well designed systems supported by the people who will deliver them.
Region-wide leadership is a ‘top-down approach’ that encourages stakeholders (clinicians, payer organisations, patients, and the public) to remain engaged in discussions around the change process.
Examples
- London reorganised its stroke services by combining top-down leadership from health authorities with bottom-up input from clinical experts. This combination resulted in system-wide ownership of the changes, which helped to overcome local resistance.
- London Cancer, a network of provider organisations, was established using several processes to support delivery of change – a consistent core leadership team, sharing responsibility with clinicians and managers across different levels of the system, and engaging actively with stakeholders.
At micro level
Leadership is central to building team cultures and behaviours that support high-quality, safe care, including creating psychological safety (where team members feel safe to speak up). One useful way of thinking about team leadership is to consider its focus – for example, on the people in the team, and on the tasks to be achieved.
Person-focused leadership engages and inspires team members to work together. It also:
- Focuses on the individual needs of team members, providing constructive feedback and
development opportunities. - Enables each team member’s skills to improve, helping them feel valued and increasing their sense of belonging and ownership of team goals.
- May become more complex when teams cover more than one profession or sector.
Task-focused leadership relates to the process by which team goals are achieved. It involves:
- A shared sense of objectives, responsibilities, and delivery to ensure that all team members are working to the same quality goals.
- Building expertise, by addressing gaps in knowledge and providing training, to increase the team’s capabilities to deliver high-quality care.
Eight top tips for governance and leadership
Eight top tips for governance and leadership – text-only version
At macro level (national):
- Use incentives carefully: Incentives can drive change but may have unintended consequences. Involve people managing, delivering, and using services in developing incentive systems.
- Consider practical and emotional burdens: Make sure the right resources (people, capacity, time) are in place to deal with the practical and emotional burdens associated with improvement efforts.
At meso level (systems and organisations):
- Prioritise quality and safety: This should be a central priority for boards. Include them on agendas, use data to support understanding of quality and safety, and dedicate resources to building expertise in these areas.
- Build a case for quality: Leaders should use both hard data (such as performance metrics) and soft data (such as patient stories) to make a compelling case for improving quality and building an improvement culture.
- Learn from others: Boards should be open to building networks with and learning from external organisations to improve their own approaches to quality and safety.
- Combine approaches: Making large-scale improvements requires combining both top-down leadership (from the board) and bottom-up approaches (from frontline staff).
At micro level (clinical teams):
- Use person-centred leadership: Leaders should focus on individuals’ needs and aspirations. Constructive feedback enhances team skills, sense of value, and encourages ownership of team priorities.
- Use task-centred leadership: Establish shared objectives, responsibilities, and ownership for quality within teams. This promotes a culture of collaboration, psychological safety, and innovation.
Practical questions
Define the problem
- What is the problem you are trying to solve? Clearly define the quality or safety issue.
Governance structure
- What level of governance will be responsible for overseeing this issue? Is it best addressed at the macro, meso, or micro level, or a combination?
- What structures and processes are in place for oversight? For example, formal governance structures (boards, committees) and informal processes (peer networks, team dynamics).
- How can transparency and accountability be ensured? Think about systems for monitoring progress, evaluating performance, and engaging stakeholders.
Performance oversight
- How will performance be measured and monitored? Are there clear mechanisms for addressing performance gaps?
Leadership
- Who will lead the initiative, and how will they inspire and engage others?
- What leadership styles will be most effective? Consider whether a transformational approach (inspiring change) or a transactional approach (focusing on rewards and performance) is most appropriate for your initiative.
- How will you empower teams and individuals to take ownership? Encourage leadership at all levels, from senior management to frontline staff, to foster a culture of continuous improvement.
Success and sustainability
- How will you measure success? Define clear success criteria and outcomes.
- How will you ensure sustainability? Consider how improvements can be maintained over time through training, culture change, and continuous monitoring.
Adaptation
- How will you adjust leadership and governance strategies as the intervention progresses?
You can download the practical questions as a printable worksheet, with space to note down your responses.
Further reading
THIS Institute | Naomi J. Fulop and Angus I. G. Ramsay
Governance and Leadership
https://doi.org/10.1017/9781009309578
The King’s Fund
What is Compassionate Leadership?
https://www.kingsfund.org.uk/insight-and-analysis/long-reads/what-is-compassionate-leadership
THIS Institute | Jill Maben, Jane Ball, and Amy Edmondson
Workplace Conditions
https://doi.org/10.1017/9781009363839
THIS Institute | Russell Mannion
Making Culture Change Happen
https://doi.org/10.1017/9781009236935
NHS Improvement
Improvement Leaders’ Guides
https://www.england.nhs.uk/improvement-hub/wp-content/uploads/sites/44/2017/11/ILG-3.4-Leading-Improvement.pdf
The Health Foundation
How can leaders influence a safety culture?
https://www.health.org.uk/reports-and-analysis/reports/how-can-leaders-influence-a-safety-culture
NHS Leadership Academy
Learning hub
https://www.leadershipacademy.nhs.uk/bitesize/
Acknowledgements
This resource was adapted from Governance and Leadership, by Naomi J. Fulop and Angus I. G. Ramsay, part of THIS Institute’s series ‘Elements of Improving Quality and Safety in Healthcare’.
Thank you to Cath Chisholm, University Hospitals of Northamptonshire, for her insightful comments and recommendations.
Download the resources


Worksheet
You can download the practical questions as a printable worksheet, with space to note down your responses.

Sketchnote
Download the sketchnote, featuring eight top tips for governance and leadership.